How to relieve male pelvic pain in 6 exercises
6 exercises to relax and assist in changing the tight holding patterns often found in the pelvic floor of males who suffer with CP/CPPS. Practicing these exercises daily in the comfort of your own home you can start to recover and relieve your pelvic pain.
List of Exercises
- Abdominal Breathing
- Adductor Stretch
- Lying Squats
- Reverse Kegels
- Pelvic Floor Stretch (PNF D2)
- Listen to music
-
Abdominal Breathing
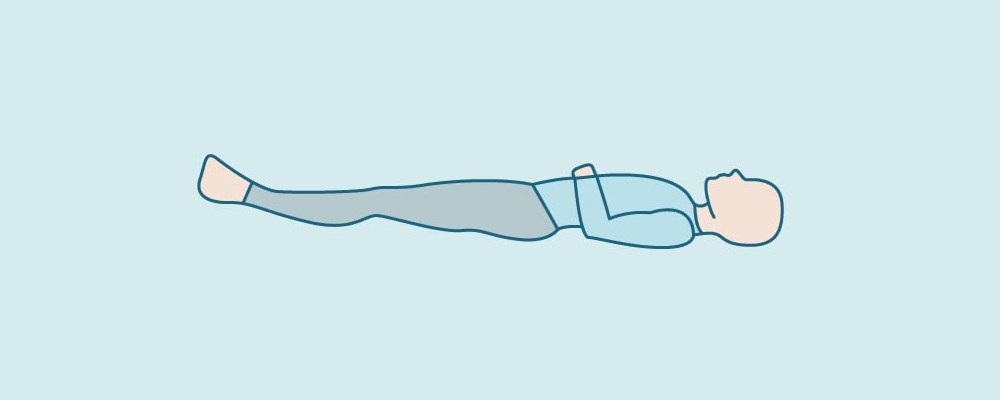
Abdominal Breathing exercise steps
- Lie on your back somewhere quiet with support under your head and knees.
- Place one hand on your chest and one on your abdomen.
- Take a slow, deep breath in through your nose. Feel your tummy rising slowly into the hand on your abdomen.
- Breathe out slowly through a relaxed mouth. Allowing your tummy to return to its starting position.
- Repeat for 5 minutes. Keep the breath slow and rhythmic (3 seconds for in, breathe, and 3 seconds for out, breathe). Don’t force it.
- This deep, abdominal breathing technique will be used in all the pelvic pain exercises. Practice this first to ensure a good foundation.
 Bevis Nathan is a specialist in pain and post-traumatic disorders, using Osteopathy, Somatic Experiencing, Breathing-and Affect-Retraining based in the UK; who agrees that abdominal breathing can drastically help to improve symptoms of CP and CPPS.
Bevis Nathan is a specialist in pain and post-traumatic disorders, using Osteopathy, Somatic Experiencing, Breathing-and Affect-Retraining based in the UK; who agrees that abdominal breathing can drastically help to improve symptoms of CP and CPPS.“Diaphragmatic breathing mimics deep sleep breathing, which promotes a relaxation response by various routes. The relaxation response as a whole will facilitate pelvic floor muscle relaxation as part of a global parasympathetic picture. Abdominal in-breath puts a gentle pressure on the pelvic floor that enhances one’s ability to become aware of it. Dissociation – lack of awareness – from pelvic floor tissues is a common problem in pelvic pain syndromes.”
-
Adductor Stretch
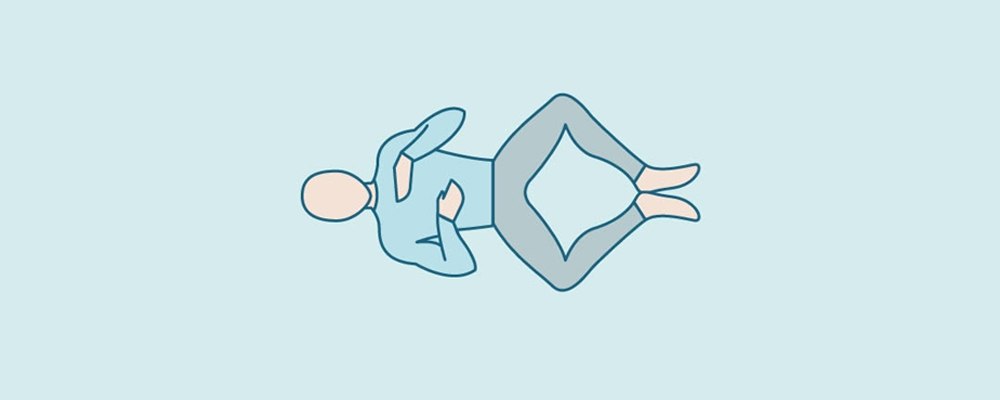
Adductor Stretch exercise steps
- Lie on your back with a pillow under your head.
- Keeping your feet together on the floor bend your knees up.
- Allow your knees to drop out to the side with the soles of the feet together. You should feel a gentle stretch on the inner thighs between the groin and inner knee. Place a pillow under each knee to provide support to begin with. Reduce the support to increase the stretch over a period of weeks.
- Follow the deep, abdominal breathing technique protocol for 2 minutes.
 Amy Stein is the author of ‘Heal Pelvic Pain’. She is the founder of Beyond Basics Physical Therapy in New York and is one of the founders of the Alliance for Pelvic Pain . Amy has a Masters and Doctorate in Physical Therapy and explains that the Adductor Stretch can help to relieve the pain caused by a direct and indirect pull into the pelvic floor.
Amy Stein is the author of ‘Heal Pelvic Pain’. She is the founder of Beyond Basics Physical Therapy in New York and is one of the founders of the Alliance for Pelvic Pain . Amy has a Masters and Doctorate in Physical Therapy and explains that the Adductor Stretch can help to relieve the pain caused by a direct and indirect pull into the pelvic floor.“Trigger points and facial tightness in the hip adductors causes a direct and indirect pull into the pelvic floor and can increase symptoms of urinary frequently, urgency and the feeling of incomplete emptying. The adductor muscles can also contribute to groin and pelvic pain.”
-
Lying Squats

Lying Squats exercise steps
- Lie on your back with your head supported on a pillow.
- Ensure your tailbone is a few inches from the wall.
- Ensure the hips and knees are bent beyond 90 degrees.
- Place your feet flat on the wall.
- Let your kneed relax and drop out to the side slightly.
- Practice the deep abdominal breathing technique protocol for 2 minutes.
- As you inhale you should feel a gentle dropping or bulging of pelvic floor between your tail and sit bones.
 Sandy Hilton has a Master of Science in Physical Therapy and a Doctor of Physical Therapy degree. Her clinical interest is chronic pain with a particular interest in complex pelvic pain disorders for men and women. Sandy runs her practice from Chicago, Illinois and says that doing deep squats can help to keep the pelvic nerves healthy;
Sandy Hilton has a Master of Science in Physical Therapy and a Doctor of Physical Therapy degree. Her clinical interest is chronic pain with a particular interest in complex pelvic pain disorders for men and women. Sandy runs her practice from Chicago, Illinois and says that doing deep squats can help to keep the pelvic nerves healthy;“Nerves, like muscles and skin, need movement and good circulation in order to get and to stay healthy. Keep the pelvic nerves healthy through deep squats. Coordinate with relaxed breathing and a sense of safety for improved confidence and function.”
-
Reverse Kegels

Reverse Kegels exercise steps
- In the squat position take a deep breath into your abdomen (as in the breathing protocol).
- As you exhale gently bear down into your back passage like you are passing wind. This is subtle and should not be forced. You should feel a gentle dropping or bulging of the pelvic floor near your tail bone.
- Repeat steps 1 and 2, this time gently bear down at the front like you are passing urine. This is subtle and should not be forced. You should feel a gentle dropping or bulging of the pelvic floor around the penis and testicles.
- Practice the above techniques for 2 minutes until you are able to feel the subtle changes in both the front and rear portions of the pelvic floor. Be patient, this may take time.
- Once you can feel this subtle change practice steps 1 to 3 with the breath and out breath.
- It should still remain subtle and gentle.
 Bill Taylor is a Fellow of the Canadian Academy of Manipulative Therapy he hold’s a Masters Degree in Physiotherapy from Queen Margaret University, Edinburgh. Over the past 15 years he has developed a special interest in the treatment of pelvic floor pain and dysfunction. He is the lead Physio at The Scottish Ballet and runs his practice from Edinburgh, Scotland. He says;
Bill Taylor is a Fellow of the Canadian Academy of Manipulative Therapy he hold’s a Masters Degree in Physiotherapy from Queen Margaret University, Edinburgh. Over the past 15 years he has developed a special interest in the treatment of pelvic floor pain and dysfunction. He is the lead Physio at The Scottish Ballet and runs his practice from Edinburgh, Scotland. He says;“Reverse Kegels or down training of the pelvic floor can be very helpful in the self treatment of CPPS. Relaxing your pelvic floor muscles is an essential component in recovery from pain and return to function. The keys to down training are visualisation and breathing control.”
-
Pelvic Floor Stretch (PNF D2)
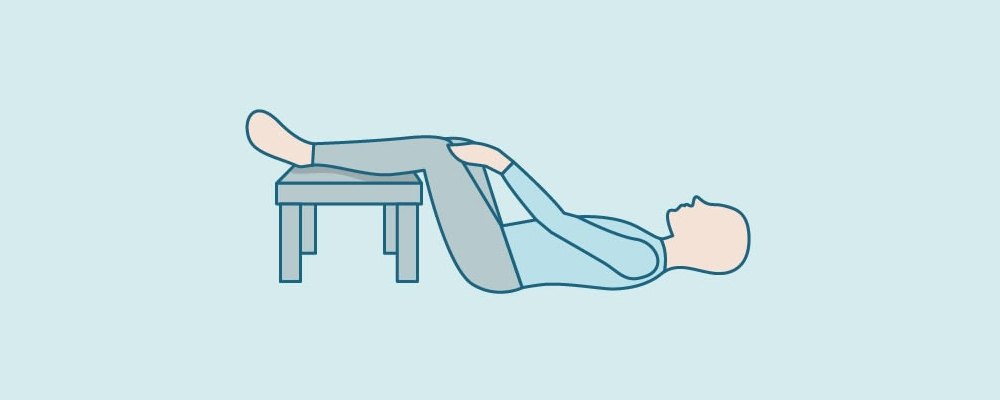
Pelvic Floor Stretch (PNF D2) exercise steps
- Lie on your back with a pillow supporting your head.
- Bend your hips and knees to 90 degrees and place your feet on a chair.
- Place your feet together and allow your knees to relax out to the side.
- Place your fingertips on your knees.
- Gently push your knees into your fingertips (using roughly 10% of your strength).
- Aim to gently push your knees up and out your ears, to where the corners of the wall meet the ceiling behind you.
- Hold for 5 seconds, relax and repeat. Practice for 30 seconds.
- You should feel a slight drop and bulge of the pelvic floor around the perineum, tail bone, penis and testicles (much like the Reverse Kegel exercise).
- Keep your stomach muscles relaxed, do not brace them. Use the abdominal breathing technique protocol to aid this.
 Stephanie Prendergast has a degree in exercise physiology and a master’s in physical therapy. She is the co-author of the book ‘Pelvic Pain Explained’ and runs 5 Pelvic Health Rehabilitation Centres in San Francisco, Berkeley, Los Gatos, Los Angeles and Lexington, MA and says;
Stephanie Prendergast has a degree in exercise physiology and a master’s in physical therapy. She is the co-author of the book ‘Pelvic Pain Explained’ and runs 5 Pelvic Health Rehabilitation Centres in San Francisco, Berkeley, Los Gatos, Los Angeles and Lexington, MA and says;“PNF D2 is a helpful exercise to help people learn how to volitionally relax their pelvic floor muscles. It involves a neurologic principle called reciprocal inhibition. This means that activation of certain muscle groups will result in relaxation of others, in this case the pelvic floor muscles.”
-
And finally… Listen to music

- Plug in you headphones
- Select your music
- Press play
- Lose yourself in your favourite tunes
 Dr Don Knox is a senior lecturer in Audio Technology at Glasgow Caledonian University. His main research interests include audio and music analysis and classification, music emotion, and music psychology, with a focus on developing multidisciplinary research into music technology for health and wellbeing.
Dr Don Knox is a senior lecturer in Audio Technology at Glasgow Caledonian University. His main research interests include audio and music analysis and classification, music emotion, and music psychology, with a focus on developing multidisciplinary research into music technology for health and wellbeing.“Listening to music can be an effective part of managing chronic pain. Studies show it can reduce perception of pain, anxiety and stress, improve pain tolerance levels, and result in a reduction of drug requirements. The ‘most effective’ music is generally positive, low arousal and bright. Music can distract the patient from persistent pain, increasing feelings of control and improving mood.”
________
By practicing the described exercises to relieve male pelvic pain daily you can help to improve your symptoms in the comfort of your own home. They can assist in building a solid foundation for the recovery from CP/CPPS and its associated symptoms. If any of these exercises recreate pain or any of your symptoms it is essential that you stop and seek professional advice. Each presenting case is unique and specific to the individual, you should therefore have the guidance and assistance of a qualified and experienced therapist to ensure a safe recovery.
If you are suffering from Male Pelvic Pain and would like to learn more about how you can relieve your symptoms, you can visit our Treatments page for more details or Contact Us directly for professional advice.
References
- Roberts RO, Lieber MM, Rhodes T, Girman CJ, Bostwick DG, Jacobsen SJ. Prevalence of a physician-assigned diagnosis of prostatitis: the olmsted county study of urinary symptoms and health status among men, Urology, 1998; vol. 51, no. 4, pp. 578-584.
- Liang CZ, Li HJ, Wang ZP, Xing JP, Hu WL, Zhang TF, Ge WW, Hao ZY, Zhang XS, Zhou J, Li Y, Zhou ZX, Tang ZG, Tai S. The prevalence of prostatitis-like symptoms in China”, The Journal of Urology, 2009; vol. 182, no. 2, pp.558-563.
- Ejike CE1, Ezeanyika LU. Prevalence of chronic prostatitis symptoms in a randomly surveyed adult population of urban-community-dwelling Nigerian males, International Journal of Urology, 2008; vol. 15, no. 4, pp. 340-343.
- Clemens JQ, Meenan RT, O’Keeffe Rosetti MC, Kimes T, Calhoun EA. Prevalence of and risk factors for prostatitis: population based assessment using physician assigned diagnoses, The Journal of Urology, 2007; vol. 178, no. 4, part 1, pp. 1333-1337.
- Wagenlehner FM, Pilatz A, Bschleipfer T, Diemer T, Linn T, Meinhardt A, Schagdarsurengin U, Dansranjavin T, Schuppe HC, Weidner W. Bacterial prostatitis, World Journal of Urology, 2013; vol. 31, no. 4, pp. 711-716.
- Collins MM, Stafford RS, O’Leary MP, Barry MJ. How common is prostatitis? A national survey of physician visits, The Journal of Urology, 1998; vol. 159, n. 4, pp. 1224-1228.
- Wise GJ. Prostatitis: myths and realities, Urology, 1998; vol. 53, no. 1, pp. 240-241.
- Mazzoli S. Conventional bacteriology in prostatitis patients: microbiological bias, problems and epidemiology on 1686 microbial isolates, Archivio Italiano di Urologia e Andrologia, 2007; vol. 79, no. 2, pp. 71-75.
- Alexander RB, Propert KJ, Schaeffer AJ, Landis JR, Nickel JC, O’Leary MP, Pontari MA, McNaughton-Collins M, Shoskes DA, Comiter CV, Datta NS, Fowler JE Jr, Nadler RB, Zeitlin SI, Knauss JS, Wang Y, Kusek JW, Nyberg LM Jr, Litwin MS; Chronic Prostatitis Collaborative Research Network. Ciprofloxacin or tamsulosin in men with chronic prostatitis/chronic pelvic pain syndrome: a randomized, double-blind trial Annals of Internal Medicine, 2004; vol. 141, no. 8, pp. 581-589
- Nickel JC, Downey J, Clark J, Casey RW, Pommerville PJ, Barkin J, Steinhoff G, Brock G, Patrick AB, Flax S, Goldfarb B, Palmer BW, Zadra J. Levofloxacin for chronic prostatitis/chronic pelvic pain syndrome in men: a randomized placebo-controlled multicenter trial, Urology, 2003; vol. 62, no. 4, pp. 614-617.
- Zhou Z, Hong L, Shen X, Rao X, Jin X, Lu G, Li L, Xiong E, Li W, Zhang J, Chen Z, Pan J, Song B. Detection of nanobacteria infection in type III prostatitis, Urology, 2008; vol. 71, no. 6, pp. 1091-1095.
- Chen Y, Wu X, Liu J, Tang W, Zhao T, Zhang J. Effects of a 6-month course of tamsulosin for chronic prostatitis/chronic pelvic pain syndrome: a multicenter, randomized trial, World Journal of Urology, 2011; vol. 29, no. 3, pp. 381-385.
- Nickel JC, Krieger JN, McNaughton-Collins M, Anderson RU, Pontari M, Shoskes DA, Litwin MS, Alexander RB, White PC, Berger R, Nadler R, O’Leary M, Liong ML, Zeitlin S, Chuai S, Landis JR, Kusek JW, Nyberg LM, Schaeffer AJ; Chronic Prostatitis Collaborative Research Network. Alfuzosin and symptoms of chronic prostatitis-chronic pelvic pain syndrome, 2008; vol. 359, no. 25, pp. 2663-2673.
- Hetrick DC, Ciol MA, Rothman I, Turner JA, Frest M, Berger RE. Musculoskeletal dysfunction in men with chronic pelvic pain syndrome type III: a case-control study, The Journal of Urology, 2003; vol. 170, no. 3, pp. 828-831

